Across busy hospitals, steam is the hidden lifeline that heats rooms, sterilizes tools, and conditions air—yet failing traps can silently waste energy, strain budgets, and complicate patient care. When even a small portion of hundreds or thousands of traps malfunction, the loss compounds into rising utility costs, unreliable service, and tougher maintenance conditions.
That backdrop explains why systematic steam trap surveys have become a hallmark of strong facility management. The U.S. Department of Energy reports typical annual trap failure rates of 15–20%, climbing to about 50% when maintenance is deferred. Proactive surveys counter that slide with data, bringing clarity to where energy goes, how risk accumulates, and which steps will pay back first.
Why Steam Trap Surveys Matter in Hospitals
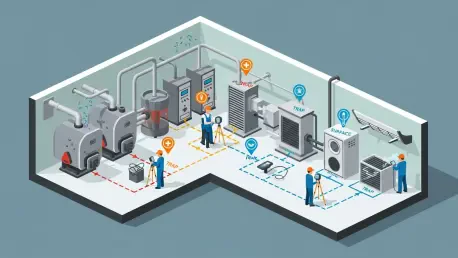
Hospitals depend on steam for heating, sterilization, and humidification, so performance dips ripple into operating rooms, labs, and patient spaces. Failed-open traps leak live steam; failed-closed traps hold condensate that can hammer equipment; both scenarios waste energy and erode reliability. Moreover, hidden leaks tend to worsen at the worst possible moment.
A best practice survey reframes the problem from guesswork to evidence. Using ultrasound and temperature differential testing under real loads, technicians confirm each trap’s condition and evaluate adjacent components—valves, strainers, checks, bypasses, and test points—to head off repeat failures. The result is a clearer picture of the system, not just a list of bad actors.
The Case for Best Practices and the Benefits Hospitals Can Expect
The strongest reasons are straightforward: control utility spend, protect clinical uptime, and cut emissions. In contrast to reactive fixes, disciplined surveys funnel scarce maintenance hours toward the highest-impact issues, while also documenting safety constraints that influence scheduling and access.
Facilities that lean into this approach typically see less energy loss, fewer unplanned outages, safer work conditions, and faster decisions enabled by credible data. Incentives can further improve the math, helping projects hit payback in under two years—often under one.
Best Practices for High-Impact Steam Trap Surveys in Healthcare Facilities
Build a Complete, Traceable Asset Inventory
Start by tagging every trap and nearby components, capturing location, application, pressure, model, pipe size, surface temperatures, installation notes, and access limits. Standard naming, floor plans, and route maps pay dividends during repairs and across the lifecycle.
Network-wide inventories have unlocked coordination at scale. For example, cataloging 9,817 traps across a large health system created shared visibility that supported bundled repair work and streamlined planning.
Use Instrumented Diagnostics for Accurate Findings
Combine ultrasound with temperature differential testing to determine whether a trap is cycling properly, leaking, or stuck. Verification of isolation valves, strainers, and check valves prevents new parts from failing early due to upstream issues.
Field crews often uncover traps that look warm yet fail open under pressure, especially on sterilizers and heat exchangers. Quantifying live steam loss for those units strengthens cost recovery and prioritization.
Identify Safety, Access, and Shutdown Constraints Upfront
Flag hot surfaces, confined spaces, above-ceiling locations, and isolation gaps before work begins. Documenting conditions that require shutdowns enables after-hours windows and coordination with infection control, avoiding disruptions to patient care.
In surgical areas, for instance, traps hidden behind ceiling tiles with limited isolation can be scheduled for targeted, off-peak outages with clear safe access controls.
Quantify Energy Losses and Model ROI Rigorously
Translate failed-trap conditions into therms or pounds of steam and then into dollars using site-specific rates. Balance survey fees, parts, and labor with incentives to present ranked recommendations by payback.
In one systemwide effort, quantified savings exceeded $2.4 million with 946,500 therms conserved and nearly $1.2 million in incentives, producing a 1.4-year ROI and a defensible plan for capital and operations teams.
Prioritize Repairs for Quick Wins and Risk Reduction
Address the biggest leaks and clinical hot spots first, then bundle medium-priority fixes to minimize mobilizations. Validate each repair with post-fix readings and update the asset record to keep the database trustworthy.
Clusters of failed-open traps on sterilizers and heat exchangers often deliver immediate reductions in gas and electric use while stabilizing temperatures critical to patient safety.
Institutionalize Data-Driven Maintenance
Set a recurring cadence—annual systemwide surveys with semiannual checks in high-risk zones. Integrate findings with the CMMS to track lifecycle and align projects with budget cycles and incentive timelines.
Over time, trending failure rates by model and service informs a smarter spares strategy and standardization on proven designs, steadily improving reliability.
Conclusion and Decision Guide for Hospitals
The evidence pointed to a simple path: treat steam trap surveys as a standing practice that merges diagnostics, safety planning, and financial modeling. Facilities that embedded this approach prioritized the right repairs, captured incentives, and reduced outages without guesswork. Next steps were clear—commit to a traceable inventory, deploy instrumented testing, price savings with site rates, and feed results into the CMMS on a set cadence—so leadership could fund what pays back first while shrinking risk across the steam network.